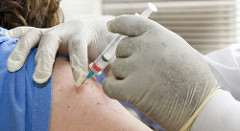
Should you be fired for refusing a flu shot?
Should you be fired for refusing a flu shot?
That’s apparently the fate of some health care workers, according to recent news reports. It is a front page story in this week’s issue of Modern Healthcare.
Health workers are also patients; the Patient’s Bill of Rights says they may accept or refuse any proposed treatment or therapy. Some have opted not to receive the flu shot.
Hospital and health company executives say they are putting the lives and health of other staff and patients in jeopardy.
Most of these health workers – nurses, physicians, aides, technicians – are still on the job. However, some are now required to inform patients of their immunization status and to wear masks over their mouths. Is this a violation of the worker’s health privacy? Or does the obligation of the hospital to protect their patients and other employees nullify the privacy argument? It’s both a public health and ethical dilemma.
Across the country, cities and states are declaring health emergencies. The CDC has officially labeled this an epidemic, and reports a vaccine shortage in some parts of the country.
Still, some health care workers say they have a right to refuse the vaccine – on scientific, religious or moral grounds. They say they’re not convinced of the vaccine’s efficacy or that vaccinating health workers leads to better patient protection. One health employees’ union even sued the state of Rhode Island over its mandate.
OSHA guidelines highlight health employees as a priority group for vaccination. They encourage employers to make the shot available, have health workers who provide direct care for sick patients use precautions, and allow for flexible and generous sick time, should a worker become ill. But these are recommendations, not mandates.
Professor Arthur Dobrin, Ph.D., teaches applied ethics at Hofstra University. He said that two basic questions need to be asked: Does the flu shot help reduce the risk of getting the disease and how great is the disease risk to the population?
If the answers are “yes” and “high” then “health workers have an obligation to get the shots. The first directive of ‘do no harm’ applies here. There may be exceptions on religious grounds but they need to be seen as just that, exceptions.”
Who’s right here? Can your employer “make” you have a certain medical treatment by threatening termination? Should it matter if you work in the health field vs. any other occupation? Do these workers have a case? Or are they being selfish and putting lives of co-workers and patients – particularly the elderly – at risk?
![]()