In recent years, “leaky gut” has become a popular phrase in health circles — often mentioned in connection with fatigue, bloating, food sensitivities and even skin conditions. But what does it actually mean? And is it a legitimate health concern or simply a wellness buzzword?
If you’ve been struggling with persistent digestive discomfort, unexplained inflammation or symptoms that don’t quite add up, you may have already encountered the term while researching support from a trusted naturopath in Perth. Understanding what’s happening inside your digestive system is the first step toward making informed, sustainable changes to your health.
What’s Leaky Gut Syndrome?
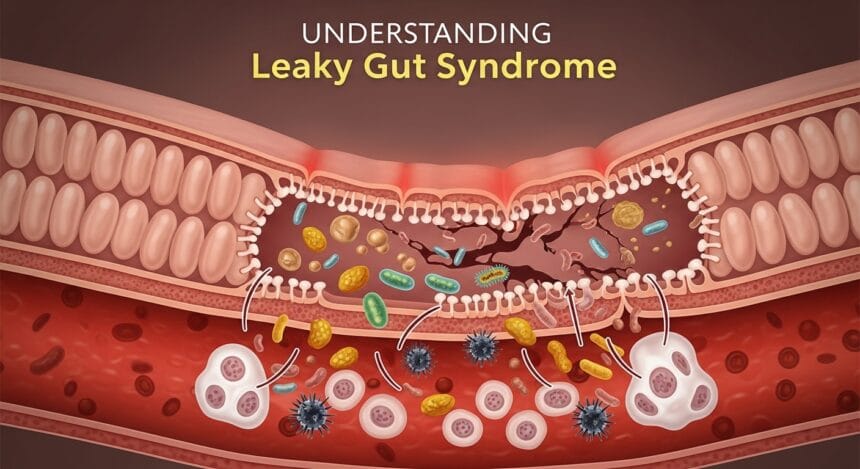
“Leaky gut” is the common name for a condition medically referred to as increased intestinal permeability. Your gut lining is designed to act as a carefully regulated barrier. It allows nutrients from digested food to pass into the bloodstream, while keeping harmful substances — such as toxins, bacteria and partially digested food particles — safely contained within the digestive tract.
The intestinal lining is made up of tightly packed cells connected by structures known as tight junctions. When these junctions become compromised, gaps can form. This may allow unwanted substances to pass through the gut wall and enter the bloodstream. The immune system can then react to these substances, potentially triggering inflammation and a range of systemic symptoms.
While increased intestinal permeability is recognised in conventional medicine — particularly in conditions such as coeliac disease and inflammatory bowel disease — the broader concept of “leaky gut syndrome” remains debated. However, many integrative and functional practitioners consider gut permeability a meaningful factor in chronic inflammatory and digestive complaints.
Common Symptoms Associated with Leaky Gut
Because the gut plays a central role in immunity, nutrient absorption and hormone balance, symptoms can extend well beyond digestion. Individuals who may have increased intestinal permeability often report:
- Bloating, gas and abdominal discomfort
- Food sensitivities or intolerances
- Persistent fatigue
- Brain fog or difficulty concentrating
- Skin issues such as eczema, acne or rashes
- Joint aches or unexplained inflammation
- Frequent infections or lowered immunity
It’s important to note that these symptoms are non-specific and can be linked to many different conditions. A thorough health assessment is essential before drawing conclusions.
What Causes Increased Intestinal Permeability?
There is rarely a single cause. Instead, leaky gut is typically associated with a combination of lifestyle, dietary and environmental factors.
- Chronic stress: Long-term stress can disrupt gut motility, alter the microbiome and weaken the integrity of the intestinal lining.
- Poor diet: Highly processed foods, excess refined sugar, alcohol and food additives may contribute to inflammation and imbalance in the gut microbiome.
- Gut dysbiosis: An imbalance between beneficial and harmful bacteria in the gut can compromise the protective mucosal layer and affect tight junction function.
- Medications: Non-steroidal anti-inflammatory drugs (NSAIDs), antibiotics and certain other medications have been shown to increase intestinal permeability.
- Underlying conditions: Coeliac disease, inflammatory bowel disease, chronic infections and autoimmune conditions are associated with compromised gut lining function.
The Gut–Immune Connection
Around 70% of the immune system resides in the gut-associated lymphoid tissue (GALT). When the intestinal barrier is weakened, the immune system may be repeatedly exposed to substances it would normally not encounter. This ongoing exposure can lead to chronic, low-grade inflammation.
Some researchers suggest that increased intestinal permeability may play a role in the development or exacerbation of autoimmune conditions. While more research is needed, the gut–immune connection is a growing area of scientific interest.
How Is Leaky Gut Assessed?
There is no single standardised test universally accepted for diagnosing “leaky gut syndrome.” However, healthcare practitioners may use:
- Comprehensive health history and symptom review
- Testing for coeliac disease or inflammatory markers
- Stool analysis to assess microbiome balance
- Functional tests designed to evaluate intestinal permeability
Importantly, diagnosis should never rely on symptoms alone. A personalised assessment ensures other conditions are ruled out.
Supporting Gut Health Naturally
Restoring gut integrity is not about a quick fix. It involves addressing the underlying drivers and supporting the body’s natural repair processes.
- Dietary modifications: Emphasising whole, nutrient-dense foods is foundational. This may include fibre-rich vegetables, quality proteins, healthy fats and fermented foods. Reducing processed foods, refined sugar and excessive alcohol can also ease inflammatory burden.
- Supporting the microbiome: Prebiotic fibres and probiotic-rich foods can help rebalance gut bacteria. In some cases, targeted probiotic supplementation may be appropriate under practitioner guidance.
- Managing stress: Stress reduction techniques such as mindfulness, breathwork, gentle movement and adequate sleep are critical for gut healing.
- Nutritional support: Certain nutrients — including zinc, L-glutamine and omega-3 fatty acids — are often discussed in relation to intestinal lining support. Supplementation should always be individualised.
When to Seek Professional Guidance
Digestive symptoms that persist or worsen should always be assessed by a qualified healthcare provider. Self-diagnosing leaky gut and eliminating large groups of foods without guidance can lead to nutritional deficiencies and further imbalance. An experienced practitioner can help you determine whether increased intestinal permeability may be contributing to your symptoms, or whether another underlying condition requires attention.
The goal is not simply to label the issue, but to restore balance and resilience to your digestive system as a whole.
The Bottom Line
Leaky gut syndrome remains a topic of both scientific investigation and clinical debate. What is clear, however, is that gut health plays a profound role in overall wellbeing. The integrity of the intestinal lining influences digestion, immunity, inflammation and even mental clarity.
Rather than focusing on a single buzzword diagnosis, a more productive approach is to support the gut through evidence-informed nutrition, stress management and personalised care. When the gut is supported, the ripple effects can extend throughout the body — improving energy, resilience and long-term health.