Consumer Operated and Oriented Plans (CO-OPs) — the stealth public option under Obamacare — were to be founded by providers, with control passed to members within a year of beginning member enrollment. There was supposed to be on

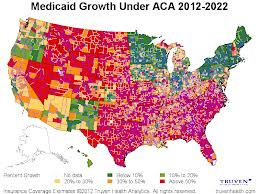
Consumer Operated and Oriented Plans (CO-OPs) — the stealth public option under Obamacare — were to be founded by providers, with control passed to members within a year of beginning member enrollment. There was supposed to be one in each state, and the idea was to provide an alternative to traditional health insurance offerings. This was something new and different, and the folks inside the Beltway figured that about a third of them wouldn’t make it. Nevertheless, the ACA committed significant sums to kickstart the effort and shore up the CO-OPs as needed. This all sounded like a fine idea until the Republican Congress called a halt to establishment of new CO-OPs after only 23 had been established, and decided to cap coverage of risk corridor payments to about 12% of the total previously budgeted. The federales ended up shorting CO-OPs to about $2.5 billion a year. Twelve of 23 CO-OPs created under the Affordable Care Act have folded, causing dislocations for members who had to scramble to find other affordable coverage. The Massachusetts CO-OP has secured some additional funding in the form of a federal loan, and the Oregon CO-OP filed a class-action lawsuit claiming the CO-OPs have been stiffed to the tune of $5 billion.
The risk corridors program represents one way in which the federales were trying to promote coverage of previously uninsured individuals and others through CO-OPs and other plans offered through the health insurance exchanges (essentially offering to reimburse health plans for a portion of enrollees’ claims experience that exceeds expectations over certain thresholds). This was intended to be a transitional program, but many of the plans that were to have been its beneficiaries seem to be mortally wounded. It is unclear at this time what the ultimate fate of the CO-OPs will be, and what the ultimate fate of the health insurance exchange plans will be. While some of the health insurance giants have expressed an interest in dropping out of the exchanges, they have also expressed concerns about the viability of their Medicare Advantage plans, and the rates for 2017 were increased (resulting in an increase in their stock prices). Perhaps funding could be found to cove the risk corridors program expenses as well. Perhaps Congress will stop trying to repeal the ACA and start trying to ensure that affordable health insurance coverage is available to all under the terms of the ACA.
David Harlow
The Harlow Group LLC
Health Care Law and Consulting