A study published on October 31 in the online open source journal NeuroImage: Clinical further blurs the boundaries of what it means to be conscious.
A study published on October 31 in the online open source journal NeuroImage: Clinical further blurs the boundaries of what it means to be conscious. Although the title, Dissociable endogenous and exogenous attention in disorders of consciousness, and the research methodology are almost indecipherable to those of us not inside the beltway of chronic Disorders of Consciousness (DoC) research, the University of Cambridge translates for us on their website.
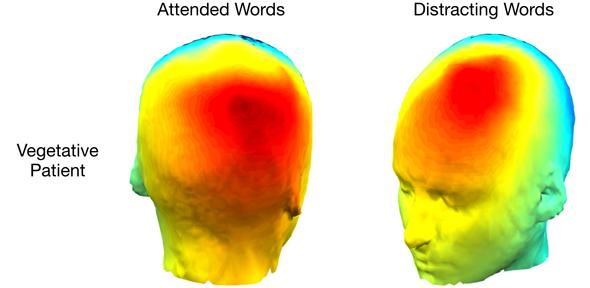
Basically the researchers, led by Dr. Srivas Chennu at the University of Cambridge, were trying to see if patients diagnosed as either in a vegetative state (VS) or minimally conscious state (MCS) could pay attention to (count) certain words, called the attended words, when they were embedded in a string of other randomly presented words, called the distracting words. Normal brain wave responses were established by performing the word testing on 8 healthy volunteers. The same testing was then applied to 21 brain damaged individuals, 9 with a clinical diagnosis of vegetative state and 12 with a diagnosis of minimally conscious state. Most of the patients did not respond to the presentation of words as did normal volunteers. But one did.
The patient, described at Patient P1, suffered a traumatic brain injury 4 months prior to testing. He was diagnosed as “behaviorally vegetative,” based on a Coma Recovery Score-Revised (CRS-R) of 7 (8 or greater = MCS). In addition to being able to consciously attend to the key words, this patient could also follow simple commands to imagine playing tennis.
Dr. Chennu was quoted as saying, “We are progressively building up a fuller picture of the sensory, perceptual and cognitive abilities in patients” with vegetative and minimally conscious states. Yes, this is true. But what does it mean if someone previously diagnosed as vegetative can now be shown to perform this sort of task? Dr. Chennu hopes that this information will spur the development of “future technology to help patients in a vegetative state communicate with the outside world.”
I think this is fascinating research and it sheds new insights into how the brain functions, but it also raises a number of important questions. For example, if I can attend to words, does it change my prognosis? Patient P1 was found to have minimal cortical atrophy. Perhaps he is just slow to transition from a vegetative to a MCS. If attending to words is associated with a better prognosis, should that make me a candidate for intensive and expensive rehabilitation? If so, who should pay for this? If I have an advanced directive that says I don’t want to continue to live in a persistent vegetative state, will this level of awareness mean I am not really vegetative. As more and more resources are poured into care for folks with severe brain damage, does it come at a societal cost? What trade offs are we making, what services are we forgoing, as we spend money developing tools to improve communication in vegetative states?
Of course no one has the answer to these questions and I suspect as researchers like those at Cambridge continue to learn more about the functioning of the severely injured brain, the more difficult it will be to clearly say what is really means to be “aware.” Stay tuned.
(image courtesy University of Cambridge)








