As we move into the dog days of summer, the sultry heat that accompanies this period of time can have us seeking out the cool oases of the beach, pools, and water parks. In addition to this, as our country continues to grapple with the coronavirus pandemic evidence is increasingly showing that participating in outdoor activities creates a lower risk than those that occur indoors. Nonetheless, as we all migrate outside whether for pleasure or necessity it is important to keep in mind that the most common form of cancer in the United States (and worldwide) is skin cancer. Around 90 percent of non-melanoma skin cancers such as basal cell carcinoma and squamous cell carcinoma are associated with exposure to ultraviolet (UV) radiation from the sun, and at least one in five Americans will develop skin cancer by the age of 70.
Thankfully, when caught early these types of skin cancers are highly curable. In particular, the Mohs micrographic surgery technique has the highest reported cure rate, with a standard skin tumor that’s being treated for the first time having a success rate as high as 98 – 99 percent. In the treatment, the cancerous tissue is methodically removed through surgery and a microscopic examination of the removed tissue is conducted, ensuring that all roots and extensions of the cancer have been eliminated. Due to the double-role a physician must play as surgeon and pathologist, physicians performing the Mohs surgery must have specialized skills in dermatology, dermatologic surgery, and dermatopathology. They have often received both basic and advanced training in the technique through residency programs, specialized fellowships, observational preceptorships, and intensive training courses.
Dr. Tim Ioannides, owner and founder of Treasure Coast Dermatology, takes pride in the fact that his dermatological practice exclusively caters to medical dermatology and specializes in skin cancer. With five locations in a county that has the second highest skin cancer rate in the United States, Dr. Ioannides is well-versed in the history and advantages of Mohs micrographic surgery. “Mohs surgery is the most advanced, precise method of removing skin cancer,” says Ioannides. “The Mohs technique has been shown to have the highest cure rate of non-melanoma skin cancers. This is especially important when treating tumors on the face, neck, and ear, where incomplete tumor removal and recurrence can be devastating.”
Below, we explore the history of Mohs micrographic surgery and break down the technique used to complete the procedure.
The Surgical Procedure
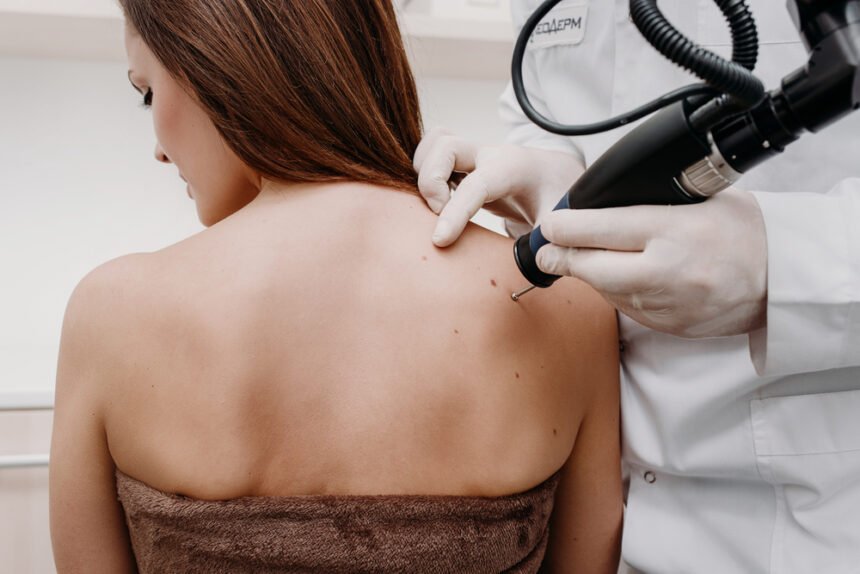
The Mohs micrographic surgery technique is a multiple-stage, single day procedure. The patient remains awake throughout the entire surgery with only a local anesthesia applied to the area in which a biopsy indicated cancerous tissue. Some skin cancers that only appear to be on the surface have roots or extensions that exist beneath the skin. Through using this technique, surgeons are able to systematically identify exactly which and how much tissue should be removed to completely rid the body of cancerous cells.
After applying the anesthesia, the surgeon will use a scalpel to surgically excise a saucer-shaped thin layer of visible cancerous tissue. Temporarily bandaging the wound on the patient, the surgeon then cuts the excised tissue into miniscule sections and uses a dye to color code each one and draws a map of the surgical site. These sections are then sent to the lab where the lab technician freezes the tissue and further cuts each one into thin horizontal slices, which are then placed on microscopic slides, stained, and covered. Using a microscope, the surgeon begins to meticulously examine the tissue on each slide, marking on the previously created map if any cancerous cells are detected.
If more cancerous cells are found, the surgeon will return to the operating room with the patient, apply more anesthesia if needed, and excise another layer of the skin in the location where the cancerous cells were located on the map. This process is repeated as many times as necessary until cancerous cells are no longer found. Once this occurs, depending on the location and size of the wound it may be left open to heal or closed with stitches. In most cases, the precise nature of the surgery means that there is no need for a skin graft or the expertise of a plastic surgeon.
History of Mohs Surgery
Mohs micrographic surgery is named after Frederic E. Mohs, MD, the founder and originator of the technique. In the early to mid-1930’s, Dr. Mohs was a research assistant who had been tasked with injecting different chemicals into cancerous rat tissue to produce specific reactions. Upon discovering that one of the chemicals — a zinc chloride solution — had the ability to freeze skin tissue, he developed a paste using the solution and found that he could excise tissue without causing bleeding where the paste was applied. This allowed him to prepare frozen sections of the excised tissue and view them under a microscope.
Dr. Mohs finished medical school and began his practice in Madison, Wisconsin and on June 30th, 1936 he performed his first procedure on a patient with squamous cell cancer of the lower lip. The procedure was originally called “chemosurgery,” a reference to the original definition of chemo meaning chemically induced due to the use of the zinc chloride paste. The paste was applied to the area where the cancerous tissue existed and after the tissue became fixed he would excise a saucer-shaped layer of it. Dividing the specimen into sections, Dr. Mohs would map out each section and using a microscope identify which sections contained cancerous cells. Due to the amount of time it took for the paste to properly fix the tissue the procedure could sometimes take days to complete, as each time cancerous cells were found the paste would have to be reapplied in the corresponding section and the entire procedure would be repeated until no more cancer cells remained in any specimens. The patient would then have to wait an additional five to seven days before a surgical repair of the wound could be performed.
Even with the amount of time the procedure took, it still held many advantages over traditional excision. Rather than removing a large amount of presumably normal skin around the tumor as a safety margin to ensure all of the cancerous tissue is removed, with Mohs’ chemosurgery technique 100 percent of the cancer could be removed while avoiding unnecessarily excising healthy tissue. This also allowed for a much better cosmetic result. However, the drawbacks of the procedure time along with the severe discomfort that came with the zinc chloride paste application made it a technique that was initially met with near universal dismay and skepticism.
In 1953, Dr. Mohs was successfully able to perform chemosurgery without the use of the zinc chloride paste. His patient had an eyelid basal cell carcinoma, and he decided to administer local anesthesia instead of the paste in order to avoid irritating the globe of the eye. No longer having to wait for the fixative to take effect, he was able to excise and examine multiple layers of tissue within one session instead of the usual wait time the paste required. As a result, he began using the new technique, although still primarily for skin cancers around the eye.
Prior to the 1960’s only one out of every five dermatologists were aware of the existence of the chemosurgery technique for treating skin cancer. However, when Perry Robins, MD, studied the procedure with Dr. Mohs, he quickly saw the great potential it had for the field of dermatology. Taking the technique to NYU, he established the first fellowship training program to teach dermatologists the skin cancer surgery. In tandem with this, Dermatologic surgeon Theodore Tromovitch caught wind of Dr. Mohs’ fresh tissue technique in 1963 and became excited by the possibilities it held. He began using the technique himself, expanding his usage from just around the eye to more and more sites on the body. By the 1980’s, numerous studies and published research showed that the fresh tissue approach was superior to using the zinc chloride paste and in the years since the vast majority of physicians have chosen to move forward singularly using that technique.
With the advent of the fresh tissue technique, the use of “chemosurgery” was no longer relevant without the use of a chemical fixative. For a period of time the two versions of the procedure were called “chemosurgery fixed tissue technique” and “chemosurgery fresh tissue technique,” but in 1974 Dr. Daniel Jones coined the term “micrographic surgery” due to the technique’s use of the microscope and the drawing of tissue maps. In 1985, the name of the procedure was officially changed to “Mohs micrographic surgery” in honor of the physician who originated it. Today, there are over 1,000 members of the American Society for Mohs Surgery (ASMS) like Dr. Ioannides who have passed the Micrographic Dermatologic Surgery (MDS) certification examination.
Due to its high rate of effectiveness and minimal invasiveness, Mohs surgery remains the golden standard for treating basal cell carcinoma and squamous cell carcinoma. In more recent years, the technique has also been evolving to treat melanoma as well. Melanoma was not previously treated using the Mohs surgery because atypical melanocytes were difficult to assess using frozen sections, but special stains have been developed that allow Mohs surgeons to see possible residual tumor that wasn’t previously visible with the regular staining.
When it comes to treating skin cancers, Mohs surgeons like Dr. Tim Ioannides are the most well equipped. With their knowledge of dermatological diseases, dermatopathology, and training to do excisions and repairs, they are able to bring the best of both worlds to the table through medical knowledge and surgical skill.