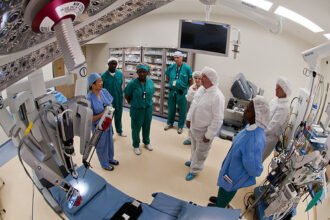
Dr Jones runs a thriving cardiology practice. Apart from being a very competent doctor and an expert in his field, there’s an all-important ingredient in his formula for success – Patient Response. Dr Jones’ team uses EMRs ( electronic medical records) which are accessible to the patient through a patient portal; and ensures that appropriate feedback is obtained after every consultation. Patients are proactively asked if they have any concerns about their treatment plan; and regular emails are sent to ensure that patients are coping well . This active involvement of patients in their treatment is what truly sets him apart from many other well-meaning doctors.
The greatest untapped resource in healthcare is the patient. More often than not, an engaged and activated patient can make the difference between healthcare success and failure.
Through Electronic Medical Record (EMR) systems, we have begun to tap that resource by prescribing information to the patient just in time to help him or her make a better health decision or to support a higher quality of self-care. Still, there is something important to consumer empowerment that is missing.
• It’s true that people can ‘pull’ a full array of medical information and decision-support tools from the Web.
• And, increasingly, doctors can ‘push’ the most relevant information and tools for each individual patient through their electronic medical record systems.
But today, there is no good way to get the patient’s voice captured within the medical record. Until we can ‘pay’ better attention to the patient’s perspectives, much of the patient’s potential will continue to go untapped. Pull, push, and pay strategies are all needed to maximize engagement.
Patient response is a new way to ensure that the patient’s voice is well heard in creating care plans, in deciding among treatment options, and in advancing the doctor-patient partnership. With patient response, patient-centered care becomes possible. Only by paying attention to the values and preferences of our patients can we achieve sufficient patient engagement to put the patient at the center of care.
Patient response defined:
• Short definition: ‘Patient response’ is the documentation of the patient’s preferences and responses to physician’s requests within the clinical record.
• Full definition: ‘Patient response’ is the documented record of a patient’s treatment, care plan, self-management, and health education preferences and responses to clinical and administrative questions, presented in the clinical record using HL7 standards, to help the clinicians support shared decision making and patient activation. Such a patient response is usually, but not always, in direct reply to a clinician’s information prescription or query to the patient.
Patients who are actively involved through information prescriptions and patient response will make better care plan decisions with their doctors and be more successful with self-management actions at home. Physicians who ask their patients to do more self-management and shared decision making can achieve better clinical outcomes, raise patient satisfaction, and reduce the cost of care. When patients are involved and informed, they can ask for the care they need, say ‘no’ to care they do not need, and do as much for themselves as possible. There is no better way to engage patients than to assure them that their voice will be heard in treatment and care plan decisions.
The Stage is set for Patient Response
Stage 1 of the Meaningful Use rules is helping to define new ways in which electronic health records (EHRs) and related health information technologies (HIT) can more actively engage patients in their care. Meaningful Use rules require that clinicians prescribe ‘patient-specific educational resources’ through their EHR systems. They also require hospitals to send discharge summaries and preventive services reminders to patients. These rules will help more patients to receive the information and tools they need to play a more effective role in their own care. This information prescription phase is a necessary step toward full patient engagement.
One-Way information is not enough
While informing patients is a key step in unlocking the patient’s potential, one-way information—by itself—is not enough. Until the physician can see, in the clinical record, the patient’s response to a query or decision aid, there is little chance that the patient’s voice will be heard. Patient-centered care will never be attained until the patient’s voice is in the clinical record and the doctor pays attention to it.
A ‘Patient Response’ is much like a medical test result
You can think of a patient response as being much like a medical test report that comes back into the record for the clinician to use in making a better diagnosis or treatment plan.
• Just as the test is done at the clinician’s request, so, too, is the patient response done in reply to a physician’s request, query, or information prescription.
• Just as the test results come back to a predictable place in the patient’s record and in an expected format that is easy for the clinician to quickly scan within a time-limited workflow, so, too, is the patient response presented in a predictable place and expected format.
• And just as an automated analysis of a medical test highlights test results that are out of normal range, so, too, does an automated analysis of the patient response flag any aspects that are important to the care plan development.
Use cases for Patient Response
Physicians are often blind to what their patients are thinking. Did I answer all of her questions? Is he planning to change his diet to prevent diabetes? Does she agree with the care plan? Did she have important symptoms that I didn’t ask about? Is she also using complementary medicines to manage her complaints? Too often there is just no time in a clinic visit to probe for the answers.
Patient response can improve the doctor-patient relationship and care outcomes by promoting empathy. With patient response, the doctor gets to learn the patient’s perspective in a short time, and the patient gets the satisfaction of knowing his voice was heard. Both enjoy the rewards of improved medical outcomes.
Here are five examples of patient response with benefits for both doctor and patient:
1. Pre-visit summaries. Pre-visit summaries are patient responses to a set of questions sent to a patient in advance of a visit. The questions are specific to the reason for the visit and interactively probe the patient’s symptoms, concerns, level of knowledge, and expectations for the visit. By starting with a succinct summary of the patient’s responses, the doctor can get to the point of the visit faster and serve the needs of the patient with more time available for education, motivation, and joint care planning. Pre-admission summaries can do much the same for improving the quality and efficiency of hospital admissions, so patients don’t have to waste time filling in multiple forms . A patient response to acknowledge patient readiness, including receiving necessary forms and consents, increases patient involvement and improves the hospital’s efficiency.
2. Patient-specific education materials and self-management learning programs. When a clinician sends the patient an information prescription or self-management program, it is important to know if the information or program is making a difference. If requested, patient response provides information back to the record regarding:
a. Whether the material was read.
b. Whether the program was completed.
c. What self-care actions were started or planned.
Patient response allows the physician to appreciate successes, empathize with struggles, and provide motivation for additional efforts.
3. Patient decision aids. Shared decision making has been shown to improve patient outcomes and satisfaction while lowering costs. However, the value of a patient’s use of a decision aid is diminished if patient insights gained from the decision aid never get back to the physician. With patient response, physicians can quickly assess if the patient is ready to make the treatment decision and what patient preferences and concerns should be considered in the decision process.
4. Medication and preventive services adherence. Patient response helps the physician know if and why a patient has either not filled or not taken a prescription medication. It also allows for fast, structured reporting of symptoms related to drug interactions or reactions. Without learning why a patient is not taking a prescribed drug, a clinician has little chance of achieving adherence. Patient response to preventive service reminders can also alert clinicians to why they are declined and whether additional information is needed.
5. Advance care planning. Advance directives are another form of a patient response. By implementing advance directives using patient response standards, this documentation becomes more accessible to the patient, more available to the clinician, and more easily transferred to those who have a need to know them.
Patient response implemented across a spectrum of uses such as those described above will enhance the doctor-patient partnership and encourages patient input to a shared care plan. And with a bit of creative thinking, we can motivate higher degrees of patient accountability by tracking patient responses.
Patient Response and Quality
Patient response supports quality initiatives in many areas of policy, reform, and health improvement. Consistent with the government’s Partnership for Care to provide better care at lower costs, patient response provides a concrete way to bring together patients and their caregivers. Patient response can validate that the patients and their families understand how to be safe from hospital-acquired disease; that the care plans are understood; and that instructions given to patients are acted upon as they transition between care settings and home.
When patients are allowed to report on their care experiences, quality-reporting initiatives are supported and customer service improvement opportunities are created. Patient response allows for patient participation in research and surveys in a meaningful way, integrated within existing workflows.
Standardizing the Patient Response
Observations and results provided to clinician orders are a fundamental feature in all EHRs. Thousands of these transactions move within any one hospital, hundreds of thousands between providers and labs, and millions across large integrated delivery systems, on a daily basis.
To maximize mainstream adoption, the existing HL7 technology standards and interoperability framework must be enhanced to integrate patient response into the clinician’s current workflow. The case for building on existing standards is a strong one:
• Ease of integration. Contextually aware patient-specific data is already available and easily transitioned to incorporate patient response.
• Existing practice. Orders, observations, and results are already widely adopted and familiar. They are easily enhanced to incorporate patient response.
• Mapped to episodes of care. Just as medical test results are matched to a specific episode of care, so the information prescription and corresponding patient response can be matched.
• Automated analysis and flagging. Automated analysis and flagging will make patient response an added blessing to the workflow of a clinician. A quick glance at the flagged responses will tell much of the patient’s story that is now available only through extended conversation well beyond today’s workflow limits.
At Last, a reason for the public to embrace EMRs
Until now, the public’s response to their $30 billion investment in EMRs has been less than enthusiastic. Their biggest concern is that someone will steal their data and they don’t yet see a compelling benefit to justify the risk. The combination of information prescriptions and patient response will dramatically change public opinion about the value of EMRs. People have concerns about electronic banking as well—but their fears are overpowered by the convenience that electronic banking gives them. In the same way, when people experience how being an informed, engaged, and respected member of the healthcare team helps them to get better care, their fears of the harms from medical data theft will be greatly moderated.
Conclusions
At this point, patient response is just a gleam in the eyes of a handful of healthcare innovators. However, the path from idea to reality can be travelled quickly. It took less than 10 years from the publication of Information Therapy to the publishing of the Meaningful Use rules that took information prescriptions mainstream. And now that information therapy has paved the way for patient response, its road can be travelled far more quickly.
To make this happen, work is needed in three areas:
1. Standards enhancement. People who have HL7 standards experience can join in an effort to modify existing standards to allow for the new functionality of patient response.
2. Policy development. People who have the ear of the government can promote the value of patient response as being essential to real meaningful use; patient-centered care; and the triple aim of better care, better health, and lower cost.
3. Use-case application development. People who have a passion for each of the patient response use cases described above can develop and test applications that can be integrated into EMR systems to achieve breakthroughs in the evolution of accountable care.
If we want patients to behave as empowered partners in their own healthcare, we need to respect them. Patient response is a great tool which allows patients to speak up—and doctors to listen!
This Chapter contributed to our book, Using Information Therapy to Put Patients First, by Leslie Kelly Hall, Senior Vice President, Healthwise ; and Don Kemper, CEO, Healthwise
HELP will be organizing its 2nd Annual Conference on Putting Patients First. The theme this time is : Using Information Therapy to Put Patients First in India.
This will be held at Nehru Centre on Sunday, 9th October’11 from 10.30 am – 1.30 pm . Mr.Ken Long , Vice President, International Operations at Healthwise, U.S.A, will be the keynote speaker and he will be talking on “What Healthwise is doing in the US to Promote Information Therapy – what we’ve learned so far”.
On this occasion, we will be releasing a book titled, Using Information Therapy to Put Patients First.