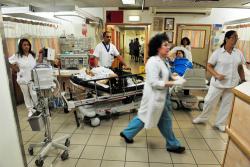
The United States healthcare system is an outlier among fellow developed nations, and not in a good way.
“We” — as in patients, private insurance, public payers like Medicare, and the taxpayers who directly or indirectly subsidize it all — pay more for healthcare as a share of GDP than our counterparts in peer countries. And we have less to show for it: higher maternal mortality, more surgical errors, lower life expectancy, and so on.
Like the healthcare system itself, the problem is vast, really an interlocking set of individual challenges that themselves seem absolutely overwhelming. We’ve seen myriad reforms in recent decades, some good and some counterproductive. We’re not going to wake up one morning and find ourselves in a place with no barriers to healthcare access and stellar outcomes across the board. Even the world’s best healthcare systems fail some patients.
Nevertheless, there’s a growing recognition among healthcare stakeholders that the status quo is unacceptable. Let’s take a look at three areas where policymakers, providers, payers, and healthtech innovators can come together to drive positive change before the decade is out.
1. Better Tools to Anticipate & Address Chronic Health Conditions
Almost anywhere you look — from agriculture to shipping to finance — you’ll find stakeholders blending increasingly powerful data analytics with deep human expertise to solve the toughest problems they face.
Except healthcare. Healthcare is woefully behind the curve in this respect.
Chuck Hollowell of Siftwell Analytics wants to change that. Drawing on decades of managed care experience and tech know-how, he and his team have developed a proprietary AI solution that analyzes population-level factors like social determinants of health as well as individual-level data to assess health plan members’ risk of developing chronic health conditions in the future. These predictive capabilities empower health plans and providers to intervene earlier in disease progression, reducing longer-term care costs while improving outcomes.
2. Faster Movement From Service- to Outcome-Based Care
The benefits of outcome-based care, also known as value-based care, have been clear for decades. The default “service-based” model encourages unnecessary or even counterproductive interventions that contribute to bloat and waste throughout the healthcare sector without meaningfully improving patient outcomes.
Healthcare stakeholders had high hopes that the Affordable Care Act would accelerate movement from service- to value-based care, yet we’ve seen only incremental progress (at best) over the past 10 years. To effect meaningful change in the coming years, more private payers need to emulate CMS’s value-based programs. And CMS needs to step up its own commitment to the transition too.
3. Better Integration of Social Determinants of Healthcare Into Care Planning and Delivery
Social determinants of health fall into five domains: economic stability, education access and quality, healthcare access and quality, neighborhood and built environment, and social and community context.
Healthcare stakeholders have limited direct control over all but healthcare access and quality, but there’s still immense untapped opportunity to better integrate all five domains into a holistic approach to health and wellness. With rare, commendable exceptions, healthcare providers and payers do a poor job of interfacing with their counterparts in social services, economic support and assistance programs, housing agencies, and educators.
This is both a systemic failing (the barriers to such coordination are simply too high) and also a practical one (healthcare stakeholders rightfully feel like they have enough else to worry about). But it’s solvable with some combination of sensible policy and best-practice changes, technological innovation, and new modes of thinking around whole-person care.
We Can Do Better
On a tactical level, “better healthcare” is a moving target because the healthcare space is constantly evolving. Treatments or pathways considered cutting-edge 30 or 40 years ago seem hopelessly outdated today.
In other words, medical innovation isn’t the problem. Inefficient delivery, outdated stigmas that impede effective care, and poor visibility into (or even understanding of) social determinants of health — these are where the opportunities for better, more inclusive healthcare lie.