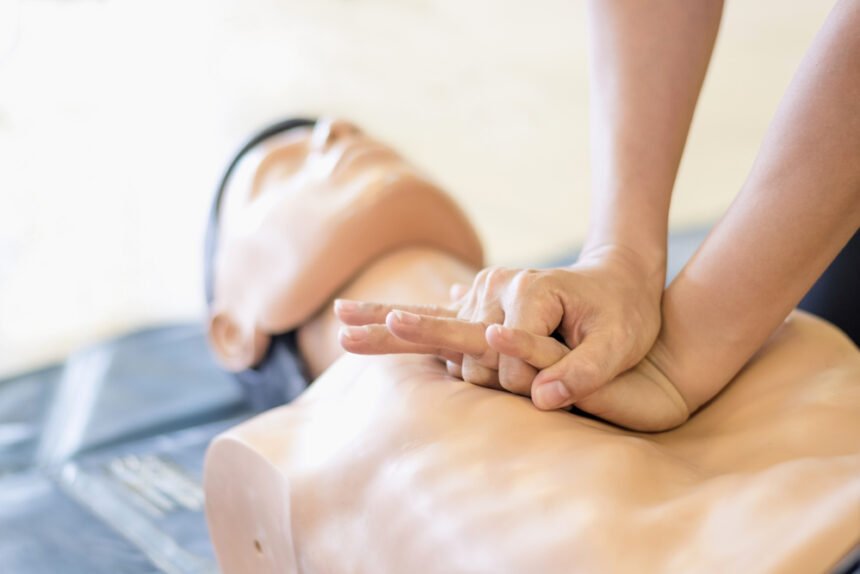
The high transmissibility and number of potential fatalities from COVID-19 has changed how healthcare providers are administering cardiopulmonary resuscitations (CPR). As a result of the pandemic, the basic procedures for CPR are no longer applicable to large swaths of patients who have contracted the coronavirus. Nowadays, frontliners are grappling at applying resuscitation and adjusting as necessary while ensuring the health of their patients and protecting themselves while providing care.
During this time, medical frontliners must review and update their CPR knowledge courses. In general, healthcare providers are advised to follow these general recommendations for managing cardiac arrest patients amid the coronavirus scare:
CPR Administration
The new rules in CPR do not apply for COVID-19 patients. The hierarchy of providing care should follow the ABC of CPR administration. You have to keep in mind that delivering CPR to the patient can generate aerosols. There should be an emphasis on sealing off the aerosols that would be produced by the patient’s airway and breathing before you even proceed on providing the necessary compressions. Never attempt to use a bag-mask for COVID-19 patients.
Before CPR, make sure the patient is wheeled in an isolated room with negative pressure, and that you have the necessary equipment within your reach, so you limit the need for going in and out of the isolated room. Prepare the following:
- Aerosol box or plastic drape
- Blood pressure apparatus
- Closed-circuit system suction device
- CPR board
- Crash cart
- Defibrillator pads
- Endotracheal tubes
- EtCO2
- Laryngeal mask airway
- Mechanical CPR device or a LUCAS if available
- Mechanical vent Stethoscope
- Pulse oximetry
- Stylet
- Surgical kit airway
- Video laryngoscope
Members of the emergency medical services must remember that during CPR, they should never bag-mask the patient if there is suspicion of COVID-19 infection. As much as possible, administer hand compressions until the advanced airway is secured. If there is an available LUCAS, they should be used the earliest time possible. Should there be available defib pads, use them instead of the traditional paddles.
Should the patient be in a prone position, administer prone CPR. According to the American Heart Association (AHA), rescuers can provide prone CPR if a supine position is not possible.
Assumption of COVID-19 Status
For the safety of all health workers, there should be an assumption that each patient that comes in the emergency room with cardiac arrest is a COVID-19 patient until they can be proven otherwise. The same assumption should be applied for dead-on-arrival (DOA) patients. Since testing for COVID-19 is still limited, it is safer to assume that every patient is positive for the virus.
Use of Personal Protective Equipment
It has been widely discussed in the medical industry that pandemics are not emergencies. Healthcare workers should not risk their lives to save another person. They must always ensure their safety first before attempting to provide care for another person. Safety first and always should be the priority. There is a need for medical frontliners to see this fight to the very end, and this is only possible if they have the necessary personal protective equipment (PPE). The complete PPE for core code team should include:
- Head-to-toe coveralls
- Face Shields
- N95 mask
- Splash gown or apron
- Double gloves
- Rubber footwear
Bystander CPR
Individuals trained to provide CPR as a bystander can attempt to provide CPR, but they should only do so if they have the appropriate PPE. If not, they should not be encouraged to provide basic care. The best thing that they can do is to provide hands-only CPR to the patient under cardiac arrest, particularly if the one to provide is a household member already exposed to the victim.
For children, the AHA guideline encourages giving both mouth-to-mouth resuscitation and chest compressions. Rescuers, however, must use a face mask to serve as a barrier when giving mouth-to-mouth ventilation.
Cardiac Arrests in COVID-19 Patients
One of the many complications exhibited by COVID-19 patients is cardiac problems. Based on the new study conducted by Chinese researchers, as much as 20% of patients who tested positive for COVID-19 developed heart failure and cardiac damage, both of which can result in cardiac arrest.
The same finding is echoed by medical experts from Italy. They noted that a good number of their COVID-19 patients would develop myocarditis, even if they were physically healthy, to begin with. The New York Times has also previously reported a patient who was initially brought to the emergency room under the assumption of a blocked artery. The patient turns out to have the dreaded coronavirus. While the focus of the SARS-CoV-2 virus is to affect the respiratory system, it seems that it is also causing damage to the cardiac system.
In these trying times, the medical frontliners are risking their lives to ensure that they save as many patients as possible. It is a daunting task to have to limit the level of care to provide for these patients. Healthcare workers should first think about their welfare. Saving their life means saving more patients against this deadly virus.