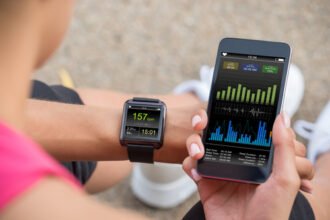
I attended the Consumer Electronics Show (CES2014), and saw hundreds of mobile health devices and applications, including activity trackers (steps, miles, stairs, sleep, etc.), vital statistics health monitors (heart rate, temperature, weight, etc.), blood chemistry monitors (glucose), and a lot more.
I attended the Consumer Electronics Show (CES2014), and saw hundreds of mobile health devices and applications, including activity trackers (steps, miles, stairs, sleep, etc.), vital statistics health monitors (heart rate, temperature, weight, etc.), blood chemistry monitors (glucose), and a lot more.
 I attended the Consumer Electronics Show (CES2014), and saw hundreds of mobile health devices and applications, including activity trackers (steps, miles, stairs, sleep, etc.), vital statistics health monitors (heart rate, temperature, weight, etc.), blood chemistry monitors (glucose), and a lot more. “Saw,” of course, being a bit of an exaggeration, as it is impossible to see it all at such a humongous event.
I attended the Consumer Electronics Show (CES2014), and saw hundreds of mobile health devices and applications, including activity trackers (steps, miles, stairs, sleep, etc.), vital statistics health monitors (heart rate, temperature, weight, etc.), blood chemistry monitors (glucose), and a lot more. “Saw,” of course, being a bit of an exaggeration, as it is impossible to see it all at such a humongous event.
At the Digital Health Summit held in conjunction with CES2014 – and in most digital health meetings and company pitches I attend – there are persistent mentions of a future where your physical, physiological and biochemical health status data gets collected on the go and gets transmitted to your doctor, either continuously or periodically or when certain pre-set boundaries are crossed. A model I often hear deals with diabetic patients whose blood glucose measurements are collected continuously and get sent to their doctor automatically. This is only one of many examples for just about anything you can measure and track.
Now, what exactly is it that your doctor is supposed to do with this information when it gets to him or her?
Assuming she gets to see your data or perhaps sees only “escapes” from your normal ranges, is she supposed to call you to do an unsolicited phone consultation or to remind you of something you’re supposed to do? Is she supposed to analyze those readings on the spot or later the same day and compare to your fitness/activity tracker data that also got transmitted? Some go as far as suggesting, and I am not making this up, that your body sensors (and those of 999 other patients) will send an immediate text message directly to your doctor’s smartphone…really?
Let’s assume for a moment that a lot of this collected and transmitted data is accurate and useful – some is, a lot is not (yet). How is all this data going to enter and be incorporated into the doctor-patient ecosystem?
 How in the world is your doctor supposed to do the scanning, interpreting and acting for the thousand-plus patients in her practice?
How in the world is your doctor supposed to do the scanning, interpreting and acting for the thousand-plus patients in her practice?
The answer, I believe, lies in the development and deployment of sophisticated decision-support systems that can use algorithms, based on clinical data and guidelines, to analyze, behind the scenes, the raw collected data and then highlight for the doctor (and patient) only outliers or exceptions at the point of care. This is both a great future state and a perfect application for the new EHR systems that are starting to get a lot of logic built into them; this is moving them from simply being record-keeping and record-sharing tools to much more valuable decision-support assistants. This capability in EHRs will relieve the need for this analysis to happen at the device end, but would require the establishment of standardized data and transmission protocols to ensure mobile device and data interoperability.
But, still, what is your doctor supposed to do with this massive amount of data and prompts, even if just exception ones?
Let’s step for a moment into today’s reality. Most doctors, unless yours is one of the few in “concierge practices”, have very little time to see and manage the patients that show up at their offices, let alone the many that don’t; the current average for a primary care office visit is around 18 minutes. The economic environment is such that doctors, especially those in primary care, must see as many patients as possible to cover all of their costs (including their astronomical education loans, overheads, insurance and administration). To compound things, there is already a scarcity of physicians in the US, only to get worse as more people enter the system because of their new coverage eligibility. Another reality is that, with few exceptions and mostly in pilot programs, physicians do not get paid for remote or virtual consultations.
With these realities in place, it is still hard to envision some future world where all of a doctor’s thousand patients will be managed, so to speak, every day. The time is simply not there, the backbone and decision-support systems are not there – yet, and the compensation mechanisms have not been worked out – yet. “Yet” is the critical word here as these are definite possibiities in a not-too-distant future.
So, not meaning to rain on the parade, but everyone designing, building and selling these mobile health technologies should focus on other features and benefits of their products first and foremost and also think of the end-to-end implications. Not that this connectivity and transmission to your doctor isn’t promising or soon valuable, but most of the utility in mobile devices and apps needs to come from some other benefit – perhaps accuracy and meaningful data would be good places to focus.
The advent of more sophisticated EHRs, of interoperability standards, and of decision-support tools in those EHRs are key to this 24/7 data-monitoring dream and opportunity. But the complexity and benefit won’t come simply from the ability to collect and transmit data – something technology is proving to be relatively easy to do (just look at the number of devices and apps). Data can’t help if the right person doesn’t see it in the right way, in the right place and in the right context. The power will come from the ability to make sense of this data and to convert it to information (presented with the right visualizations at point-of-care) that doctor and patient can use for decision-making that will lead to improved clinical outcomes and health overall.
(images: mobile health / shutterstock; health technology / shutterstock)