 Ghana faces some serious challenges when it comes to healthcare delivery.
Ghana faces some serious challenges when it comes to healthcare delivery.
 Ghana faces some serious challenges when it comes to healthcare delivery.
Ghana faces some serious challenges when it comes to healthcare delivery.
As the Austrian Red Cross points out, although the country has a population of nearly 23.5 million people, there are only 1,439 health care facilities, unevenly distributed across the country.
Additionally, roads are difficult to traverse, and transportation, particularly to rural areas scarce.
Add to the above difficulties a nursing shortage–more nurses leave than graduate each year.
In short it is often lack of access to medical care, rather than poor medical care itself, that impedes Ghana’s progress.
Enter mobile health.
Striking, mobile access is gaining ground rapidly. Projections are that 82% of Africans will have mobile access by 2014.
It is just such access–and what it can accomplish–that is changing the face of healthcare in Ghana
Unlike the individual monitoring. tracking, and personal interactions with clinicians via applications in developed countries, mobile health in Africa focuses on “improving the efficiency of healthcare workforce and systems.”
Four major mobile health projects currently operating in Ghana demonstrate this focus.
#1: Sene PDA Project
The first mobile project in Ghana, the PDA project was initiated in the Sene District in 2004 to improve treatment at initial levels of care.
The use of PDAs (as opposed to more primitive systems of record keeping) provides a tool for tracking and locating children who fail to finish the immunization process. The Community Health Officers at the first level of service delivery register children receiving immunizations, provide them with a unique identification number, and record their addresses for home visits or follow-up care.
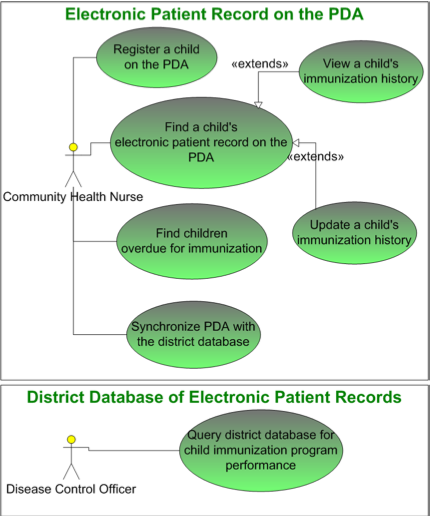
At each community visit the Officer makes to an outreach clinic, this registry instantly provides the names of the children to be vaccinated as well as which vaccines they have already had and those they still require.
The Policy Planning, Monitoring, and Evaluation Division of the health service assert that the drop-out rates for the vaccine against Diphtheria, whooping cough, Tetanus, Hepatitis B and H. influenza infections) dropped from 5.3% to 1.8% since the program was initiated.
The project was such a success that it has been replicated across the country, and PDAs are being phased out in favor of smartphones.
It t may have been the first to use mobile technology to improve healthcare in Ghana–but it is far from the last.
The Millennium Villages mhealth project moved the arena from vaccinations specifically to supporting rural health in general.
#2 Millennium Villages mhealth projects
The Novartis Foundation and the Millennium Villages Project joined forces with the Ministry of Health and the Ministry of Communications in Ghana, National Health Insurance Agency Ghana, Ghana Health Service, and Ghana Medical Association, to make accessible mobile technology to improve the quality of primary health services, particularly in rural areas.
Initially the Millennium Villages project provided an ambulance for Bonsaaso, in the Ashanti Region of Ghana.
But the maternal death rate did not go down, since women couldn’t communicate with ambulance dispatchers about their locations due to unreliable phone lines.
Mobile handset producer Ericsson, together with mobile telecommunications firm Zain, cooperated to install Internet access and mobile phone coverage throughout the area. They gave free phones to health workers and sold them to villagers for $10 each.

The introduction of mobile phones has made a tremendous difference in maternal women’s survival. With those phones given out by Ericsson, for the first time women can call ambulances in cases of emergency–and ambulance drivers can reliably receive the calls and reach the area of need.
Before cell phone and internet technology were introduced to the village in 2006, around 20 women a year died in childbirth. In 2008, after the mobile program began, not one died.
An even more innovative component of Millennium Villages is the Ghana telemedicine project. As the Novartis Foundation explains, in Bonsaaso there are only seven health centers for 32,000 people, requiring long travel, often over unpaved roads. It can take hours for a patient to reach a clinician, and then the wait time can be long enough to be dangerous.
This project focuses on minimizing unnecessary referrals to congested centers, and utilizing consultations via mobile phone so local heath care providers can gain the requisite knowledge to treat patients within their own communities.

A teleconsultation center has been set up, manned by physicians working at the main hospital.
“Now,” claim the proud funders, “health workers, nurses and other personnel are able to engage in structured consultation with doctors at the district hospital, as a result reducing unnecessary referrals and allowing for immediate support in the event of medical emergencies.”
Along similar lines the program has created ChildCountPlus application. Utilizing the mobile phones, the community health workers collect and synthesize data about their patients, with a particular focus on children and malnutrition.
Their ongoing goals are to register every child under five into the database, screen them for signs of malnutrition every 90 days, and monitor them for the three major causes of child death: malaria, diarrhea, and pneumonia.
In Millennium Villages where screening programs for malnutrition have been enacted, rates of malnutrition (assessed by ‘stunting,’ or a low height for age ration, indicating chronic malnutrition) have decreased more rapdily than in locations without the intiative.
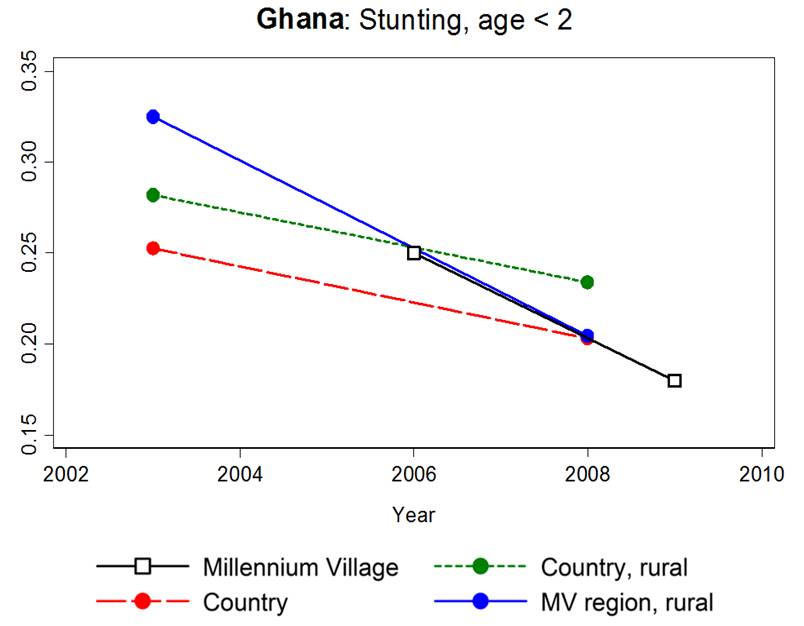
Sub-Saharan Africa accounts for 90% of malaria deaths world-wide, resistant to many on-the-ground efforts to combat it. Crucial malaria medications would run short in certain areas, leading to epidemics, while elsewhere the medicine went to waste.
A method of accounting for medicine stockpiles and ensuring the right amounts of treatment were in the right areas was needed–and mobile access supplied the technology to match up medication and demand.
SMS For Life was first piloted in Tanzania, utilizing SMS messages to keep track of anti-malarial supplies and prevent shortages.
In fact, the program went so well in Tanzania that it was rolled out in 2011 in Ghana.
Developed by the Ghana Health Service in conjunction with the Swiss Tropical and Public Health Institute, Roll Back Malaria, and Greenmash, this initiative uses mobile phones, SMS messages and electronic mapping technology to collect and share information about the location of crucial anti-malaria treatments.
This enables the Health Service to re-distribute medicines as needed, preventing shortages and unnecessary deaths.
#4 MOTECH
In Ghana, 450 mothers died per every 100,000 live births in 2008.
The Mobile Technology for Community Health (MOTECH) initiative was launched in July 2010 in the Upper East Region and in April 2011 in the Central Region, to combat maternal illness and death.
A partnership between Ghana Health Service, Grameen Foundation and Columbia University’s Mailman School of Public Health, and funded by a grant from the Bill & Melinda Gates Foundation, the initiative’s goal is to utilize mobile phones to improve healthcare for expecting mothers in rural areas.
Their project Mobile Midwife is aimed at improving care for the expecting mothers among the rural poor, utilizing voice or text messages to provide important health information during pregnancy and encouraging women to seek care. After birth, information on vaccinations and management of childhood diseases is sent.
MOTECH provides an example of the work Mobile Midwife does:
- On Tuesday, Nurse A enrolls patient B in messaging with preferences
- Patient B is enrolled for Pregnancy Informational messages starting at week 11
- Preferences for Patient B include Language English (although local languages are options), Format SMS (voice mail is a choice, as well), with delivery on Monday, Wednesday and Friday at 6 PM.
- On Wednesday at 6 PM, an SMS message will be sent to Patient B’s phone . . .including information in English related to week 11 of a pregnancy
Of course there are other factors, but Mobile Midwife has played a role in the fact that, at last count, the maternal mortality rate had dropped to 210 per 100,000 live births.
Find out a bit more about MOTECH’s goals and accomplishments with this short video:
Where mHealth initiatives have focused their energies, they have made a significant difference–one that makes their efforts stand out against the general healthcare landscape.
For example, according to Unicef, the percent of “under-fives with suspected pneumonia receiving antibiotics, 2006-2010,” an area not yet addressed by mobile health, is a paltry 24%. Additionally the “under-fives with diarrhoea receiving oral rehydration and continued feeding, 2006-2010” is only 45%.
But. . . .the immunization rates for children, an area that has been addressed in the mHealth platforms, range from 94-96%, and “antenatal care coverage, At least once, 2006-2010,” also part of an mHealth initiative, is 90%.
With a will, a way, a funding source, a mobile network–and reliable access to it–dedicated people can change the face of healthcare, and save millions of lives.
That is the miracle of mobile health.
To read other posts in this exclusive ongoing series, please visit the Mobile Health Around the Globe main page.
And if you have a Mobile Health Around the Globe story to tell, please email me at joan@socialmediatoday.com









