Just three weeks ago, I wrote about sign posts on the road to connected health adoption. That post was meant to help readers appreciate the subtleties of a changing environment. A turn of phrase by a senior executive or thought leader can easily be missed if you’re not listening carefully.
Just three weeks ago, I wrote about sign posts on the road to connected health adoption. That post was meant to help readers appreciate the subtleties of a changing environment. A turn of phrase by a senior executive or thought leader can easily be missed if you’re not listening carefully. In this case, a senior executive I work with signaled a change in thinking from ‘healthy skeptic’ to ‘fear of missing out (FOMO)’, by making the statement, “We know [connected health] is going to be a big part of care delivery so we had better start our plans to scale it.”
The healthy skeptic demands data incessantly, to the point where you suspect the ‘more data’ requests are really a polite way to say no. When convincing the healthy skeptic, you bring reams of data. You build logical arguments. When approaching the FOMO attitude, it’s more about enabling experience, assuming that the concept is valid and that eventually we’ll get the economics right. Let’s plan more pilots. Let’s learn by doing.
This is such a liberating signal for any innovator — and I’ve been hearing it a lot lately. I got this same signal from a homecare executive recently. In another example, the CEO of a company I advise intimated to me that his potential customers are no longer asking for clinical proof points as part of their due diligence on his product.
As William Gibson said, “The future is here, but it’s not evenly distributed.” As a bit of a reality check, I also received an email from a colleague who oversees innovation at one of the larger health plans. His query to me: “How do you get doctors to adopt remote patient monitoring?” and adding, “We’re not making much progress with this.”
I in no way mean to declare victory and announced my retirement, but this change in the conversation is worth paying attention to.
What might be driving this change? Many factors, I’m sure.
There is the ubiquity of mobile technology in general. When all decision makers see the power of the tool in their hand every day (not to mention the addictive nature of the technology), it is much harder to be skeptical.
There has also been a lot in the news lately about both connected health and new payment models, the latter being a driver for adoption of the former.
The Secretary of U.S. Health and Human Services (HHS) is on record saying that by 2018, 50% of Medicare payments would be risk-based. Just a few weeks later, she announced a new ACO model that will become available in 2016. The details are sparse, but notably, there will be the opportunity to take more risk, but reap more reward. Also, there will be more opportunities to encourage the use of telehealth. Health leaders know that 2018 is not far away, so we had better get planning now!
The other announcement from the Centers for Medicare and Medicaid (CMS) that will drive telehealth adoption was the new chronic care management code that came out in January 2015. This code allows physicians to bill for 20 minutes per month of non-face-to-face time spent on chronic care management. This is an ideal set up for encouraging population health and remote patient monitoring.
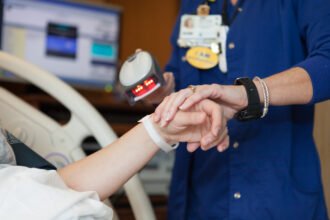
Yet another recent announcement contributing to FOMO was last week’s flurry of activity from Apple. By now, most folks believe that the Apple Watch will probably not have immediate ‘care of illness’ implications, as it seems more targeted to fitness and health. However, wearables is now a hot concept. This paves the way for thinking around monitoring of vital signs in the home, as well as mobile communication with patients.
And then there is the highly touted Apple ResearchKit. I’m not sure how this will shake out. My colleague Kamal Jethwani astutely noted that the lack of rigor around which individuals can sign up for which studies may significantly add to the burden of data analysis. Another bright commentator noted that patient self-reported data is subject to all kinds of bias. So it’s too early to tell.
But, think for a minute like an executive. You have information coming at you in an avalanche. You are used to reading headlines and instinctively sensing trends. If you read the headlines about ResearchKit (not to mention the brand-name institutions that have already signed on to use it) and didn’t think too hard about it, you’d have to conclude, “This is a big deal. We’d better get on the stick.” Next thing you know, that organization is scrambling to quickly develop a strategy for mobile health and patient engagement.
Suddenly, we are buzzing past all of that skepticism and the endless requests for data, and instead are focusing on how we’d better get moving – faster.
Perhaps these recent events are more than sign posts, but are putting us on the fast track on the road to adoption!